Pelvic Pain
January 7thPelvic pain or dysfunction within the pelvic floor muscles is likely to impact you or someone close to you at some point in your life. It is estimated that 1 in 6 men in Australia are currently experiencing pelvic pain and that persistent pelvic pain is prevalent in roughly 15-25% of women. Pelvic pain can feel debilitating at times and is commonly associated with other conditions affecting the reproductive system, musculoskeletal system, neurological and gastrointestinal system. It is also commonly linked with other symptoms such as incontinence as well as systemic diseases such as endometriosis. Some symptoms associated with pelvic pain could include: lower abdominal pain, SIJ pain, pubic pain, gastrointestinal upset, pain with bowel movements, pain with intercourse and a feeling of pressure or heaviness in the lower abdominal area.
Due to the design of the pelvic floor muscles that stretch like a hammock within our pelvis from our tail bone to our pubic bone as well as the role they play in stabilising your spine alongside your deep abdominal muscles, lower back muscles and diaphragm, it is not uncommon to see pain in other parts of the body such as the lower back and hips.
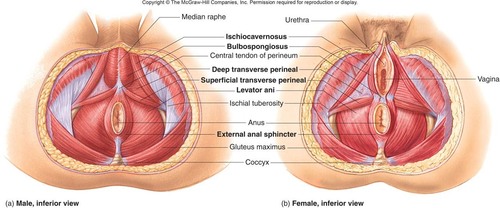
Male + Female Inferior Pelvic Floor View 2023 Quizlet Inc
PELVIC PAIN THE MULTIDISPLINARY APPROACH
One of the key things when addressing pelvic pain is to assess the pain itself as well the other symptoms or conditions that might be contributing. Keeping that in mind, it is usually collaboration between different practitioners such as a GP, pelvic floor physiotherapist and an exercise-based practitioner that allows for both symptom relief and long-term solutions for pelvic pain. A key consideration is to look at assessing the function of the pelvic floor muscles both from an internal perspective by a qualified pelvic floor specialist as well as externally by looking at movement patterns and the ability to contract and relax the pelvic floor.
A misconception I commonly see in clinic with patients is focusing only on the contraction phase as they were instructed they needed to “improve their core strength” without having an ability to relax in a gradual and controlled manner.
Another common pattern is patients seeing great progress with their pelvic floor contractions but then struggling in the next step of tying that together functionally in their day-to-day movements, with pain persisting when they try to get back into exercise or aggravating activities.
PELVIC PAIN + PILATES
One of the most evidence-based treatment protocols for pelvic pain or pelvic floor dysfunction is Pilates. Pilates is great for assisting with issues such as incontinence, pelvic girdle pain, low back pain, pelvic organ prolapse, chronic pain patterns associated with endometriosis as well as during pregnancy and the postnatal period. It can also be a great tool to use both pre and post-surgery in the abdominal/ reproductive area such as after gynaecological or prostate surgery.
The practice of Pilates has a strong focus on creating a connection between the mind, body and the pelvic floor muscles to build knowledge and awareness of how your pelvic floor functions. Through awareness we can then focus on building strength in the area as well as help to minimise any musculoskeletal contributions to the pain. As the pelvic area is key for helping to distribute load throughout the body and for stability, it is also important to look at building strength through supporting areas such as the deep abdominals, lower back and glutes.
PELVIC PAIN + MASSAGE
As well as using movement as a means of treatment, manual therapy focusing on relieving surrounding areas can also be beneficial to reduce pain symptoms. As a massage therapist and Pilates instructor, some common things I might focus on are releasing through the lower back and hips as well as adding in breathing exercises into some deep stretches or yoga poses. As pelvic pain is usually multifaceted, the approach to treatment must always be unique and specific to the individual. Your body may respond to some forms of treatments better than others and different aspects of treatment might change as you progress through your journey to ideally being pain free in the long term.
Due to the complexity of nerve innervation in the area, interplay of different muscles, as well as other conditions in other body systems, if you are experiencing pelvic pain it is recommended to seek out expertise from a health practitioner. A treatment plan at Kinematics will always be individualised and could include a combination of hands-on treatments, clinical based Pilates classes, a home exercise program and if necessary, a referral out to a pelvic health physio who can complete an internal assessment.
At Kinematics we are all about the collaborative approach and highly encourage that if you are experiencing pelvic pain to communicate any other symptoms of concern so we can give you the most holistic approach to improving your health + performance.

